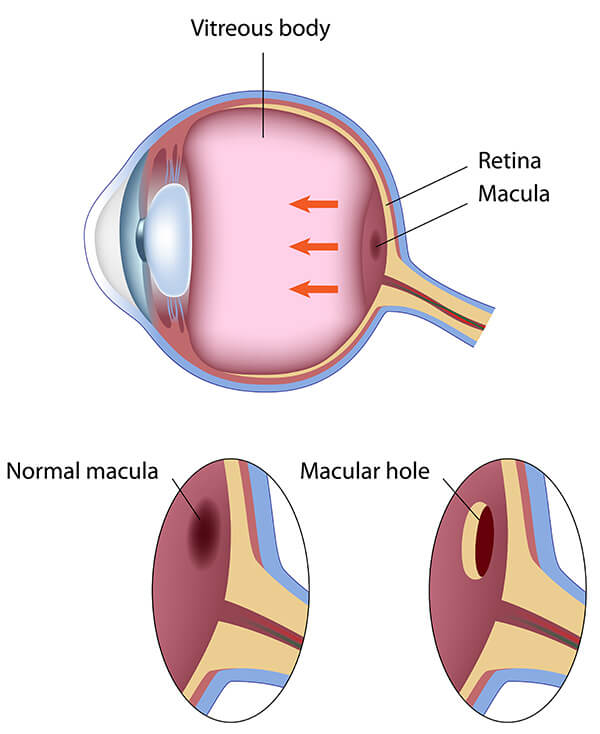
In the central portion of the retina is a small area called the macula. It provides all of the sharp central vision for activities such as reading and driving. If this area is damaged, the central vision can be affected.
Macular holes may occur as the result of age-related traction on the macula, from trauma or inflammation, from diabetic eye disease or from other factors. The hole results in progressive central vision loss.
Symptoms
Patients who develop macular holes most commonly notice a gradual decline in the central (straight ahead) vision of the affected eye. The decline can occur as blurring, distortion and waviness and a dark spot in the central vision. The size of the macular hole and the stage of its development affects the severity of the symptoms. In some cases, the other eye compensates enough that the patient notices no vision loss until they cover the good eye. The peripheral or side vision remains unchanged.
Diagnosis
Optical coherence tomography (OCT) is the most effective tool for diagnosing, staging and managing macular holes. The imaging technology delivers high resolution imagery using specific lighting to help differentiate holes from other similar conditions.
Treatment
Macular holes can be closed with an operation called vitrectomy. Macular hole surgery is usually an outpatient procedure, and eye drops will be needed after surgery. Other treatment options are used for specific macular hole conditions and sizes. Your doctor will discuss with you surgery, recovery and your individual case in greater detail.
Prognosis/Recovery
Recovery from surgery (vitrectomy) can take several weeks and is successful in the majority of patients with some or most of lost vision regained.





